There is a common condition reported in aged people termed “Frailty”. Clinically, it is defined as “a state of increased vulnerability resulting from aging-associated decline in reserve and function across multiple organ systems such that the ability to cope with everyday or acute stressors is compromised”. In other words, there is a decline in the physiology and functions in the body due to age that makes a person susceptible to health issues. This geriatric condition is linked to many causes to an overall lowering of energy levels, activity, endurance, and strength. While it is not a disability, it can up the risk of disability. In the presence of morbid conditions that affect physical and mental health such as high blood pressure, diabetes, or cardiovascular disease or affected cognition, the risk of frailty is higher.
Frailty is seen in the form of affected balance, gait, and awareness leading to falls. There are other signs such as a fluctuation in the patient requiring assistance some times while sometimes he/she is on their own along with fatigue, infections, and weight loss.
A major cause of the condition is attributed to chronic inflammation. The term “Inflammaging” has been introduced to describe the inflammation leading to aging. The presence of TNF-α, interleukin-6 (IL-6), and C-reactive protein (CRP) in even healthy aged people are independent predictors of mortality. Frail patients show alterations in the hematologic and inflammatory systems such as higher levels of fibrinogen, IL-6, factor VIII, D-dimer, leukocytes, and CRP and lower levels of hemoglobin and vitamin D. high levels of IL-6 and TNF-α are associated with lowered muscle mass, strength and physical performance such as walking.
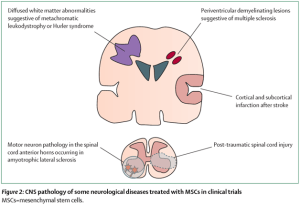
The major interventions for frailty are comprehensive geriatric interdisciplinary assessment followed by treatment and exercise. There is a decrease in the population of stem cells inside the body with age. Thus, frailty is associated with altered or damaged stem cell niches. This brings in the possibility of stem cell-based- regenerative medicine for frailty in aging. Mesenchymal Stem Cells (MSCs) lack major histocompatibility complex (MHC)/human leukocyte antigen (HLA) class II molecules to hence, evade the immune system upon transplantation. MSCs by their property of immunomodulation to lower the levels of cytokines associated with inflammation such as TNF-α, interleukin (IL)-1β, IL-6, and CRP.
The administration of allogeneic bone marrow-derived MSCs were tested in frailty in a phase I and phase II clinical trial, CRATUS (NCT02065245). In the phase I non-randomized, dose-escalation study, 15 patients with frailty according to the Canadian Study of Health and Aging (CSHA) frailty index received allogeneic MSCs. No serious adverse effects were reported while an evident increase in the six-min walk distance was seen at 3 and 6 months with lowered levels of circulating TNF-α levels significantly decreased at 6 months in all treatment groups. 30 patients with frailty received MSCs in the randomized, double-blinded, dose-finding Phase II study. There were no serious adverse effects while an improvement was seen in the 6-min walk test, short physical performance exam, forced expiratory volume in 1 s, and even the female sexuality quality of life questionnaire. The levels of activated T cells and TNF-α levels in the serum and the intracellular TNF-α in the B cells were lowered showing the promise of MSCs to lower inflammatory biomarkers-the major culprit behind frailty.
Thus, by targeting inflammation, MSCs can emerge as a cure for aging or frailty-to improve the quality of life in the aged population.
References:
Chen X, Mao G, Leng SX. Frailty syndrome: an overview. Clin Interv Aging. 2014; 9():433-41.
Schulman, I. H., Balkan, W., & Hare, J. M. (2018). Mesenchymal Stem Cell Therapy for Aging Frailty. Frontiers in nutrition, 5, 108. https://doi.org/10.3389/fnut.2018.00108