Sepsis refers to the loss of regulation of the host response to an infection. Not only is it considered the most frequent cause of death in hospitalized patients but it also accounts for an expenditure of US$24 billion per year. According to a study published in 2020 by scientists Rudd and team, close to 48·9 million people suffered from sepsis globally with 11·0 million sepsis-related deaths accounting for 19·7% of all global deaths in 2017. Though much has been uncovered about this clinical condition, accurately quantifying and treating sepsis still remains a challenge.
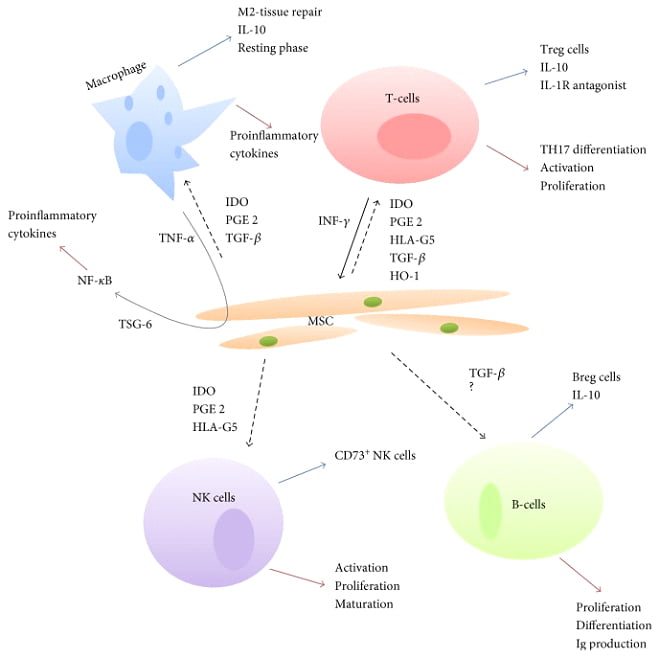
As mesenchymal stem or stromal cells (MSCs) have been shown to modulate the immune system, their use in the therapeutic treatment of a sepsis-a condition associated with aberrant regulation of the immune system is being explored.
2013-published research showed that the administration of bone marrow MSCs in caecal ligation and puncture (CLP) mice models improved the survival of the animals. Additionally, the phagocytic activity of neutrophils was increased with lowered bacterial counts in peritoneum and blood with an overall improvement in the damage to the liver, spleen and kidney (Hall et al, 2013).
In another study, CLP-induced sepsis mice models received MSCs derived from the skin of newborn mice (dermal stem cells). The symptoms and the course of the sepsis were lower in the case of animals that received the stem cells against the controls over the 10-day period of study. There was also a lowering of the cytokines involved in inflammation such as IL-1 and IL-6 (Wang et al, 2015).
Research in 2015 showed promising results in the use of adipose tissue-derived mesenchymal stem cells in mice models of toxic shock syndrome induced by staphylococcal enterotoxin A. The 40-hour mortality was lowered in the group administered MSCs to 73% from 87.5% in the controls. Additionally, the levels of cytokines involved in inflammation such as INF-γ, TNF-α, IL-6, and IL-2 were lowered due to the MSC treatment (Asano et al, 2015).
The anti-inflammatory and immunomodulatory effects of MSCs coupled with their promise in clinical trials open up the path of treating sepsis using stem cells.
References:
Lombardo, E., van der Poll, T., DelaRosa, O., & Dalemans, W. (2015). Mesenchymal stem cells as a therapeutic tool to treat sepsis. World journal of stem cells, 7(2), 368–379.
Kristina E Rudd, MD, Sarah Charlotte Johnson, MSc, Kareha M Agesa, BA et al (2020) Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study. Lancet; 395: 10219: 200-211.
Wang Y, Tan L, Jin J, Sun H, Chen Z, Tan X, Su Y, Shi C. Non-cultured dermal-derived mesenchymal cells attenuate sepsis induced by cecal ligation and puncture in mice. Sci Rep. 2015 Nov 20; 5:16973.
Horák, J., Nalos, L., Martínková, V., Beneš, J., Štengl, M., & Matějovič, M. (2017). Mesenchymal Stem Cells in Sepsis and Associated Organ Dysfunction: A Promising Future or Blind Alley? Stem cells international, 2017, 7304121.
Hall SR, Tsoyi K, Ith B, Padera RF, Lederer JA, Wang Z, Liu X, Perrella MA. Mesenchymal stromal cells improve survival during sepsis in the absence of heme oxygenase-1: the importance of neutrophils. Stem Cells. 2013;31:397–407.
Asano K, Yoshimura S, Nakane A. Adipose Tissue-Derived Mesenchymal Stem Cells Attenuate Staphylococcal Enterotoxin A-Induced Toxic Shock. Infect Immun. 2015 Sep; 83(9):3490-6.